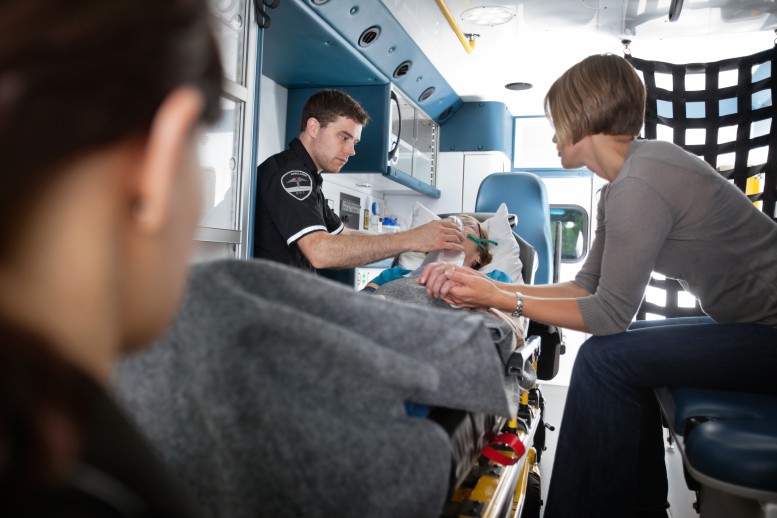
Speak Up: Making EMS a Necessary Service
By Rhonda Baliff | August 25, 2017
I spent 12 years as a volunteer EMT and quite frankly, the struggles haven’t changed for emergency medical services. In fact, it’s getting harder. In smaller communities there is often no tax support for emergency services. On top of that, a study from UC Berkeley found that of the more than 16,000 EMS workers in California, most are working very long hours without a meal break, for low pay and dealing with high injury rates. EMTs are now working in coordination with hospitals and even nursing facilities and home health providers.
EMS needs a voice like other vital services we rely on every day. As one of the most critical services in our community, these concerns must be heard in order to receive adequate funding.
So how do we make sure EMS has the dollars it needs to get to patients?
Break the Billing Nightmare
Billing is a major obstacle. Most of the country is considered rural in terms of land, but it only houses 19 percent of the U.S. population. In those rural areas, volunteers and their department often can’t afford to hire someone to specifically handle billing. So EMTs are doing the same critical paperwork someone is responsible for in the acute setting, all while responding to emergency calls. In addition, many EMTs are not trained to know the proper billing codes.
Here’s where things go from bad to worse for EMS. Industry average denial rates on reimbursement for EMS-provided services are more than 30 percent. In many EMS organizations, a volunteer EMT is then tasked with resubmitting the paperwork while keeping up with daily critical care calls. As an industry, there must be advocacy for better training for these submissions, fewer initial denials via more scrutiny of insurance company practices, and ultimately greater revenue for these departments. The need for this critical service isn’t going away, and a focus to improve billing should be part of the solution.
A Growing Need for EMS
No one questions the need for garbage pick-up, police, or fire departments. All are necessities for a civilized, functioning society. Yet, EMS is not funded at nearly the same levels. Despite this lack of public consideration, there is an increasing pressure on the critical services that EMS provides.
The trend to age in place at home is increasing with the number of people in the U.S. 65 and older from 35 million in 2000 to more than 49 million in 2016. As our older population grows, we have more people that are sicker and experiencing more emergency situations at home. The Wisconsin EMS Association (WEMSA) says it has seen an increase in the number of emergency calls per year in their larger municipalities. While organizations like WEMSA are critical voices in the state and federal legislative processes in securing the funding EMS needs to continue providing these life-saving services, we need more. Their members can play an integral part in state legislation where there are strong organizations like WEMSA, but we need broader coverage representing communities across the country.
Staff to Address the Entire Continuum
Survival rates are a key performance measure, and it of course will continue to come under pressure because of our country’s growing baby boomer population coupled with the uncertainty that comes from volunteer EMS teams. One solution is taking root. Hiring a full-time staff that can also deliver in-home services through paramedicine takes some of that burden off budgets while enhancing the full continuum of care. That’s why some legislative dollars have been put forward for research on paramedicine with the understanding the entire continuum is impacted by EMS. In New Mexico, a pilot paramedicine program witnessed a three percent reduction in readmission rates. We must view EMS as a partner in improving outcomes across the full continuum of care. More opportunities to influence how and where we use EMS providers across a broader range of the health care system should be investigated and rolled out across our country.
How are you changing the EMS is viewed and supported in your community?
In order to be successful and thrive, you need a strategic partner and supply source who understands your business and everyday needs in emergency medical services. We’re here to help.
Rhonda Baliff
EMS Division Sales Manager
Rhonda Baliff is the EMS Divisional Sales Manager at Medline. Prior to this role, Baliff was a divisional sales manager in the post-acute segment. Baliff spent 12 years as a volunteer emergency medical technician (EMT) in her hometown’s rescue squad in Wisconsin. Prior to joining Medline, Baliff was the regional manager of practice development for Aspen Dental. Baliff attended Southwest Technical College in Fennimore, Wis., where she received her Associates in business administration and management.