Listening to the Story Behind the Data
By Martie Moore, RN, MAOM, CPHQ | August 28, 2017
Gloves are like a second skin for clinicians but that hasn’t always been the case. It wasn’t until 1992. That’s when OSHA published its Bloodborne Pathogens Standard which required employees to use gloves, and other forms of personal protective equipment, to help limit occupational exposure. This marked a major shift in healthcare.
Yet, this “second skin” has taken gloves from revolutionary to simply utilitarian today — a means to an end. But hands are telling us a deeper story.
What’s Happening Under the Glove
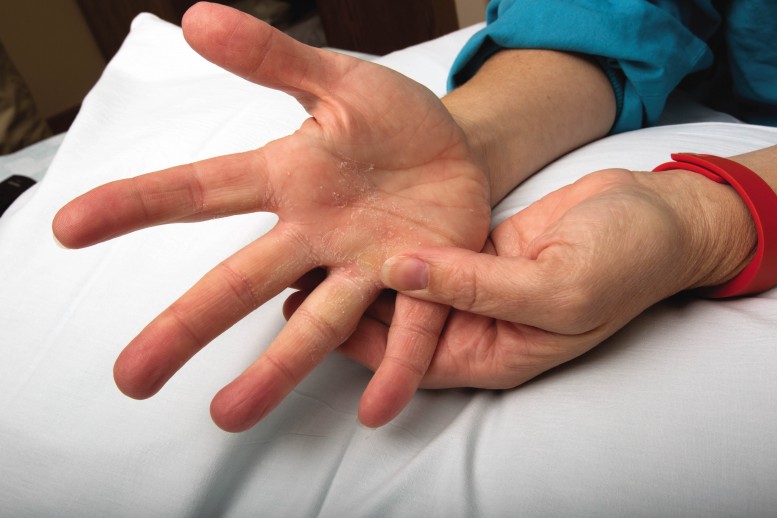
If you think about what’s happening underneath there, it’s hot, it’s moist and many times, it sets up the perfect scenario for skin breakdown. Medline commissioned insights among 240 nurses across the country to see how the condition of hands impacts hand hygiene and clinician well-being. It revealed nearly all respondents (94 percent) overwhelmingly experience skin irritation on their hands with a whopping 79 percent saying the condition of their hands impacts their quality of life. Some may say with more than four million professionally active nurses in the U.S., it’s not a significant representation. But I challenge you to ask yourself, does this data ring true?
When I looked at it, what I saw was that as a nurse leader, I really didn’t think about what was happening within my workforce when it comes to the condition of skin under gloves, and the conversation that wasn’t happening around me on a daily basis.
We have to change our thought patterns to no longer see gloves and the use of gloves as utilitarian. They have to be tools to preserve clinician skin so they can continue caring for others. They have to be tools to help the nurses have the healthiest, intact skin as possible because we also now understand that when skin breaks down and becomes cracked, it can harbor a potential transmission of disease.
We Need a Wake-Up Call
If we think about the role hands play, and we think about how much they’re in different kinds of environments like soap and water, or an alcohol-based hand sanitizer, or literally in blood and body fluids utilizing gloves; hands play an incredible role in healing in healthcare. And when we start to step back from that and think about the role that hands play, it’s almost like this aha moment where you go, “How can it not be that hands are not hurting or skin is not damaged given the type of work they go through and the type of environmental chemicals that hands are exposed to?”
In my career, I did have a scenario where I had about five nurses ready to leave their profession because of the condition of their skin. That was my aha moment that we can do this differently. We have to do this differently.
Data is like truth telling because people see it as an opportunity to share their story. They want decision makers to understand and they also want help. They don’t want their painful hands to continue impacting their quality of life and livelihood.
Data tells a story. For leaders of clinicians, infection prevention and employee health, what will it take to listen?
Martie Moore, RN, MAOM, CPHQ
Chief Nursing Officer
Martie L. Moore, RN, MAOM, CPHQ, is the chief nursing officer at Medline. As CNO, Moore develops forward-thinking, solution-driven clinical programs, as well as new products and educational services. Prior to joining Medline, Martie was the chief nursing officer at Providence St. Vincent Medical Center in Portland, Ore. Under her leadership, Providence St. Vincent earned a third and fourth designation for Magnet.
